LLight
Member
- Joined
- May 30, 2018
- Messages
- 1,411
New post summarizing some data already posted here:
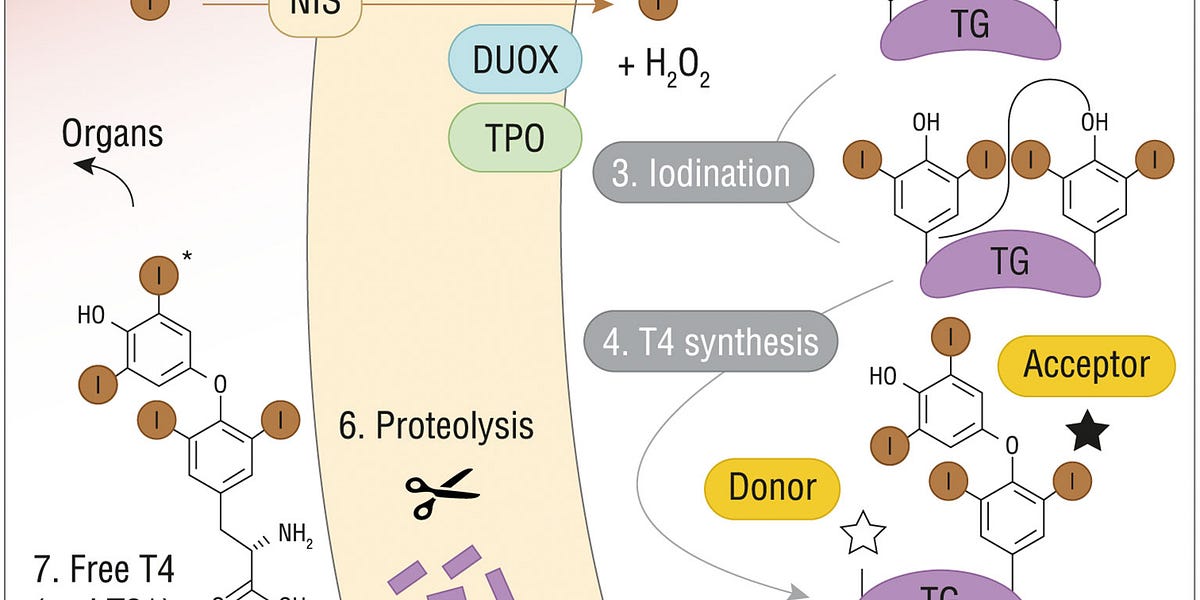
Thus, water restriction (or deuterium depletion) could lead to a TSH decrease while keeping thyroid hormones levels maintained or increased. The TSH decrease could be explained by an increase in vasopressin, which could play the role of a TSH surrogate and stimulate bile acids synthesis and thus the conversion of T4 to T3 in peripheral tissues.
Another explanation could be that hyperosmolarity itself, by activating the NFAT5 transcription factor which would upregulate the uptake of inositol by the thyroid, or activating the CREB3L1 transcription factor, would increase the sensitivity of the thyroid gland to TSH and optimize thyroid hormones output.
Upping intake of inositol, selenium and intermittently restricting water intake to achieve hyperosmolarity may improve the function of the thyroid system.

- There exist theoretical arguments allowing us to hypothesize that hyperosmolarity, induced by water restriction for example, could facilitate the synthesis of thyroid hormones while potentially lowering the requirement for TSH stimulation.
- Rats (with an animal model of hypothyroidism) put under water restriction got an increase in their T3 levels, bringing them almost back to the control group’s levels.
- It was found that, in rabbits, vasopressin itself seems to play a role similar to TSH regarding thyroid hormone synthesis.
- Two studies on rats found that water restriction or deuterium depleted water (which might be interpreted by the body as water restriction) tend to lower TSH levels.
- Finally, bile acids could be related both to the TSH and metabolic rate of tissues involved in thermogenesis, but are also related to water homeostasis as the bile acid TGR5 receptor (along with the FXR transcription factor) is involved in kidneys’ function. From this data, we can hypothesize that a TSH decrease itself could boost T3 systemic levels as it might increase bile acids synthesis and thus peripheral deiodinase enzymes.
Thus, water restriction (or deuterium depletion) could lead to a TSH decrease while keeping thyroid hormones levels maintained or increased. The TSH decrease could be explained by an increase in vasopressin, which could play the role of a TSH surrogate and stimulate bile acids synthesis and thus the conversion of T4 to T3 in peripheral tissues.
Another explanation could be that hyperosmolarity itself, by activating the NFAT5 transcription factor which would upregulate the uptake of inositol by the thyroid, or activating the CREB3L1 transcription factor, would increase the sensitivity of the thyroid gland to TSH and optimize thyroid hormones output.
Upping intake of inositol, selenium and intermittently restricting water intake to achieve hyperosmolarity may improve the function of the thyroid system.