Giraffe
Member
- Joined
- Jun 20, 2015
- Messages
- 3,730
Information I read about insulin secretion and blood glucose levels in response to a meal seem contradictory and twisted to support a specific dietary doctrine. I searched a bit and found a study on insulin response after a high-protein meal. - "Test meals consisted of 500 g of either cooked ground beef or chicken liver calculated to contain 8.0 and 10.2 g of leucine, respectively." - Protein-rich indead!haidut said:So, assuming one keeps a steady dietary supply of sucrose (or some other type of sugar), wouldn't the constant presence of glucose in the blood stream keep insulin chronically elevated too? I have read various, and often contradictory, statements from Peat about the whole blood sugar and insulin thing. Often, he says that it is important to always keep blood glucose up to keep cortisol at bay and metabolism high. Of course, this means insulin would be elevated chronically too. On insulin, Ray sometimes says it is a good hormone responsible for anabolism and keeping tumor growth under control. At other times he has said that elevated insulin is not a good thing. So, I am bit confused about the overall dietary guidelines. Should we try to keep blood sugar elevated all the time but at a certain stable (and reasonable) level, which would imply higher (but stable insulin), or should we do pulse feeds which would temporarily bring insulin up to shuttle the glucose to the muscles and then insulin goes down and the body runs on glycogen from the liver?
http://www.ncbi.nlm.nih.gov/pmc/article ... 7-0135.pdf
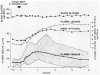
In average plasma insulin peaked after one hour, and it was still elevated at the fourth hour in some tests. In one subject "plasma insulin had not returned to control levels by the eight hour."
Could it be that our understanding of the role of insulin is misled?
From the paper I linked...
"It is unlikely that the increases in blood glucose either caused or contributed importantly to the increases in plasma insulin observed."
Ray Peat ...
It was this sort of experiment that led to the concept of "glycemic index," that ranks foods according to their ability to raise the blood sugar. David Jenkins, in 1981, knew enough about the old studies of starch digestion to realize that the dietitians had created a dangerous cult around the “complex carbohydrates,” and he did a series of measurements that showed that starch is more “glycemic” than sucrose. But he simply used the amount of increase in blood glucose during the first two hours after ingesting the food sample, compared to that following ingestion of pure glucose, for the comparison, neglecting the physiologically complex facts, all of the processes involved in causing a certain amount of glucose to be present in the blood during a certain time. (Even the taste of sweetness, without swallowing anything, can stimulate the release of glucagon, which raises blood sugar.)
http://raypeat.com/articles/articles/glycemia.shtmlInsulin is important in the regulation of blood sugar, but its importance has been exaggerated because of the diabetes/insulin industry. Insulin itself has been found to account for only about 8% of the "insulin-like activity" of the blood, with potassium being probably the largest factor. There probably isn't any process in the body that doesn't potentially affect blood sugar.
Glucagon, cortisol, adrenalin, growth hormone and thyroid tend to increase the blood sugar, but it is common to interpret hyperglycemia as "diabetes," without measuring any of these factors. Even when "insulin dependent diabetes" is diagnosed, it isn't customary to measure the insulin to see whether it is actually deficient, before writing a prescription for insulin. People resign themselves to a lifetime of insulin injections, without knowing why their blood sugar is high.
By the way, I searched Ray Peat's references, the study I linked is not mentioned on his website.