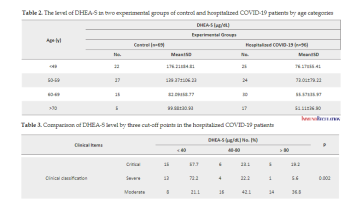
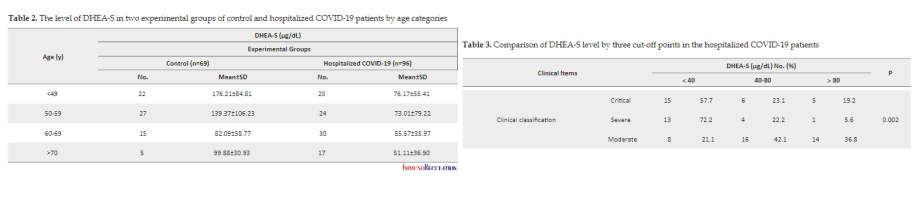
DHEA levels are low in people hospitalized with covid
(when controlled for age group - so its not just that people older aged have lower DHEA levels, but within the age group also DHEA levels are ~50% less in people hospitalized vs controls,
and the drop in DHEA levels correlates with severity)

* all hospitalized people had around or <80 mcg / dl.
of them DHEA levels <40 = 48% death rate, 40-80 = 30% death rate, >80 = 20% death rate,
(i would want DHEA levels >100 at least)
(DHEA levels drop <100 in some people over age 50, or in people with colitis / gut inflammation (partly because of cortisol medication but also due to other things like lower fat intake or absorption, DHEA goes down the most out of hormones on low fat diet))
Activation of Immune Function by Dehydroepiandrosterone (DHEA) in Age-Advanced Men
DHEA given to men in their 60s boosts immune cell counts & actively a big amount
(basically the immune loss seen in old age is mostly down to the drop in DHEA levels - which restores when you restore it)
And as a bonus
DHEA-S inhibits human neutrophil and human airway smooth muscle migration
DHEA has anti inflammatory effect in the lungs, inhibits neutrophil migration to sites of inflammation.
(excessive neutrophil migration is the mechanism behind lung damage in viral infections)
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC1750969/
So DHEA has a dual pro-immunity anti-inflammatory action , which i dont see a lot
Effects of DHEA (Dehydroepiandrosterone) on Host Virus Interactions

"Because DHEA is a native steroid that has been used clinically with minimal side effects, the utility of DHEA in the therapeutic modulation of acute and chronic viral infections including acquired immune deficiency syndrome (e.g.,HIV) deserves intensive study."
(when controlled for age group - so its not just that people older aged have lower DHEA levels, but within the age group also DHEA levels are ~50% less in people hospitalized vs controls,
and the drop in DHEA levels correlates with severity)
* all hospitalized people had around or <80 mcg / dl.
of them DHEA levels <40 = 48% death rate, 40-80 = 30% death rate, >80 = 20% death rate,
(i would want DHEA levels >100 at least)
(DHEA levels drop <100 in some people over age 50, or in people with colitis / gut inflammation (partly because of cortisol medication but also due to other things like lower fat intake or absorption, DHEA goes down the most out of hormones on low fat diet))
Activation of Immune Function by Dehydroepiandrosterone (DHEA) in Age-Advanced Men
DHEA given to men in their 60s boosts immune cell counts & actively a big amount
Activation of immune function occurred within 2–20 weeks of DHEA treatment.
When compared with placebo, DHEA administration resulted in a:
. 20% increase (p < .01) in serum IGF-I,
. The number of monocytes increased significantly after 2 (+45%) and 20 (+35%) weeks of treatment.
. The population of B cells fluctuated with increases at 2 (+35%) and 10 (+29%) weeks of treatment.
. B cell mitogenic response increased 62% (p < .05) by 12 weeks.
. Total T cells and T cell subsets were unaltered. However, a 40% increase in T cell mitogenic response, 39% increase in cells expressing the IL-2R(CD25+), and 20% increase in serum sIL-2R levels were found at 12–20 weeks of DHEA treatment, suggesting a functional activation of T lymphocytes occurred.
. NK cell number showed a 22–37% increase by 18–20 weeks of treatment with a concomitant 45% increase (p < .01) in cytotoxicity.
There were no adverse effects noted with DHEA administration.
(basically the immune loss seen in old age is mostly down to the drop in DHEA levels - which restores when you restore it)
And as a bonus
DHEA-S inhibits human neutrophil and human airway smooth muscle migration
DHEA has anti inflammatory effect in the lungs, inhibits neutrophil migration to sites of inflammation.
(excessive neutrophil migration is the mechanism behind lung damage in viral infections)
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC1750969/
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC7026770/The steroid hormone DHEA has been shown to be beneficial in animal experiments of trauma or sepsis [24-27]. Previous studies by our group revealed that these beneficial effects are concomitant with a reduced amount of infiltrating neutrophils in distinct tissue sites, for example, lung tissue [28]. As neutrophil extravasation is mainly caused by adhesion molecules, we suggested that DHEA has a specific effect on adhesion molecule expression.
In the present study we demonstrate that DHEA has distinct in vitro effects on surface expression patterns of adhesion molecules of endothelial and neutrophil origin. This result is interesting because a concentration of 10-8 M resembles the physiological DHEA concentration. The strongest effects of DHEA occurred with a DHEA concentration of 10-8 M compared to a concentration of 10-5 M
However, these effects could not be detected when DHEA was applied after LPS challenge. Thus, DHEA was not able to reverse inflammatory effects in vitro. Nevertheless, we do conclude that one mechanism of action by which DHEA exerts protective effects is via the modulation of adhesion molecules as DHEA alone did affect adhesion molecule expression. In this experimental setting, cofactors that are essential for the modulation of inflammatory responses in vivo might have been missing.
we found that modulating effects triggered by DHEA treatment were always opposite to the effects induced by LPS.
(probably the main mechanism why DHEA is helpful in colitis, where DHEA levels drop by 50% - helping lower the excessive neutrophil damage)DHEA inhibited leukocyte adhesion to the endothelium in venules of the inflamed mouse cremaster muscle. Importantly, in a model of lung inflammation, DHEA limited neutrophil recruitment in a DEL-1–dependent manner.
In conclusion, DHEA restrains neutrophil recruitment by reversing inflammation-induced downregulation of DEL-1 expression. Therefore, the anti-inflammatory DHEA/DEL-1 axis could be harnessed therapeutically in the context of inflammatory diseases.
So DHEA has a dual pro-immunity anti-inflammatory action , which i dont see a lot
Effects of DHEA (Dehydroepiandrosterone) on Host Virus Interactions
Administration of DHEA alone was also associated with enlargement of the spleen germinal centers which suggests stimulation of the B lymphocyte dependent areas.
Protection against lethal infections by coxsackievirus B4 with DHEA wasobtained if the hormone was administered in a) the diet or by subcutaneous injection.
our initial results demonstrate that in order for DHEA injected S.C. to have an antiviral effect, the hormone must be administered in a lipophilic vehicle
The results demonstrate that administration of a single dose of DHEA (S.C) to* db/+ mice resulted in a significant protection from coxsackie virus B4 mortality for at least 11 days [by restoring native immunity] [no significant extra benefit if DHEA levels already good]Effects of DHEA (Dehydroepiandrosterone) on Host Virus Interactions
"Because DHEA is a native steroid that has been used clinically with minimal side effects, the utility of DHEA in the therapeutic modulation of acute and chronic viral infections including acquired immune deficiency syndrome (e.g.,HIV) deserves intensive study."
Attachments
Last edited: